Units 10 & 11 Horizon Business Village
1 Brooklands Road, Weybridge, Surrey. KT13 0TJ.8am - 6pm Weekdays
8am - 1pm SaturdaysCOVID-19 Combat Kit

Imagine this. You develop a cough and a fever and worry that you have COVID-19 infection. So you call your GP who asks you how high your temperature is. You do not have a thermometer in the house and cannot give a definite answer. You feel hot but do you actually have a fever?
Your GP asks you if you feel short of breath. Your chest does feel a little tight but is that due to the infection or is it because you are feeling a little anxious about having COVID-19?
It has been estimated that 40-70% of us are going to get a COVID-19 infection. All UK GPs have now moved to telephone and video consultations. If you have a cough, fever, runny nose or sore throat, they will not be asking you to attend the clinic for assessment. That means that they cannot make the same accuracy of diagnosis that they are used to when they were able to see patients face to face.
If your symptoms are severe, your GP will ask you to call 111 or go to the Accident and Emergency department of the local hospital. You do not really want to go to the hospital unless you really need to. You will be putting yourself at greater risk of infection and further burdening the health service.
In this situation, having some basic medical devices at home can allow you and your doctor to get a more confident assessment of your condition.
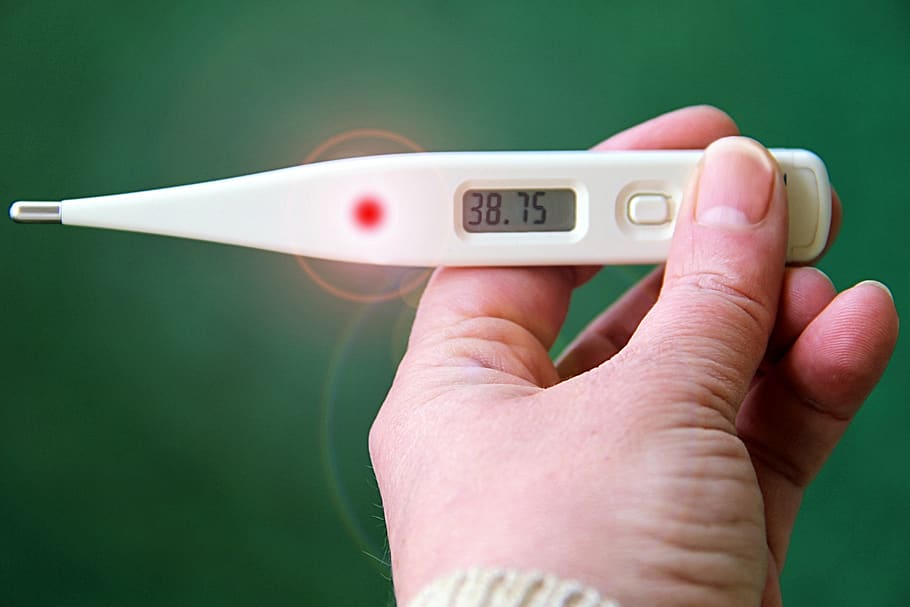
Every house should have a thermometer
A body temperature over 37.5 C (99.5 F) is a fever.
There are a number of thermometers that you can purchase which are inexpensive and will do the job perfectly well.
Ear thermometers
The ear thermometer that you are used to seeing in your GP surgery is used because it has disposable covers. That avoids cross-infection from one patient to another. This type of thermometer can be purchased for home use and can be used for different family members. However, in this crisis it is becoming increasingly difficult to find.
Digital thermometers
A more practical solution may be to use a standard digital thermometer. It is widely available and much more cost-effective for an item that you are going to use only occasionally.
The way to use this thermometer is to place the tip beneath the tongue until it beeps. However, you will need one thermometer for each household member because of the risk of spreading infection.
The other, less reliable method, is to place the tip of the thermometer in the closed armpit. Remember you will need to add 1 C to the reading if you are going to do it this way to get the correct reading.
Forehead thermometers
The infrared forehead thermometers are newcomers to the market and are accurate if used properly. These are the ones that you may have seen used in airports. The are used by scanning people’s foreheads from a distance of a few centimetres.
Advantages are that they can be used for more than one person and can be used in babies
The other type of forehead thermometer is the strip that is used for babies. It works by direct application to the baby’s forehead. The colour change of crystals in the strip tells you the temperature.
Consider getting a pulse oximeter
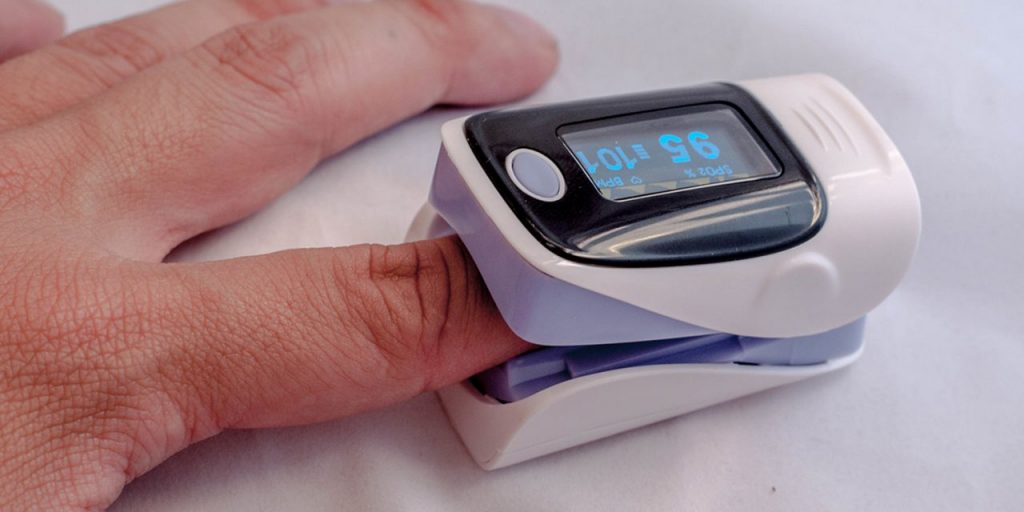
People who have severe COVID-19 infection get a severe type of chest infection that worsens their breathing. A pulse oximeter is vital to check oxygen levels in the body to assess the severity of that infection. This is more important for people who already have longstanding chest problems such as asthma.
A pulse oximeter is a device that measures the percentage of oxygen in your blood. It also shows your pulse or heart rate.
Everyone should have an oxygen saturation of 100%. However, the standard pulse oximeters only have 2-digits so they will give a maximum reading of 99%.
Normal heart rate is between 60 to 100 per minute.
Adult patients with severe COVID-19 infection will have an oxygen saturation of 93% or less. Their breathing rate (number of breaths per minute) will also be 30 or more per minute. Please note that these figures are different for children and a doctor should be notified more urgently in their case.
Of course, you should not wait until your oxygen saturation reaches such a low level of 93%. You should seek medical attention for any level of 95% or less, or if you feel that your breathing is getting worse.
The price of these devices has also gone up in recent weeks from an average of £35 to ridiculous prices of £90 or more from profiteering. Waiting time for delivery has also gone up.
Most asthma sufferers are already familiar with using peak flow meters to assess their breathing ability. These simple devices can give an indication from day to day if your asthma is deteriorating.
The best way to use a peak flow meter is to check your level when you are feeling well and note it somewhere. Then when your breathing feels worse, you can compare it your normal levels. Click here to read how you can use a peak flow meter effectively.

Paracetamol or ibuprofen?
I was in a supermarket a couple of weeks ago when I came across the over-the-counter medication section. It was completely empty, except for shelves of ibuprofen!
This is another sign of the times and the power of social media. It was after the French health minister made the claim that ibuprofen worsens the condition of COVID-19 patients.
Thankfully, we now have real evidence to the contrary rather than one person’s opinion. King’ College London have conducted research showing that ibuprofen is perfectly safe to use. So you can now go and get some medicine which is in good supply!

Should you be wearing a mask?
At the current time, there is no government advice for everyone to wear a protective mask. Such advice is only for those at high risk such as health and social care workers.
For everyone else, the standard advice remains:
Stay at home
– Only go outside for food, health reasons or work (but only if you cannot work from home)
– If you go out, stay 2 metres (6ft) away from other people at all times
– Wash your hands as soon as you get home
– Do not meet others, even friends or family.
– You can spread the virus even if you don’t have symptoms.
Summary
Many of us are likely to get COVID-19 infection. For most of us, we will get mild to moderate symptoms. Only a minority will get severe infections needing hospital admission. There also a proportion of us who will have infection without any symptoms at all.
Primary care doctors are working remotely so they are not in the best position to assess your symptoms as they used to be. It is, therefore, important that we all take more responsibility for our health. By taking sensible measures we can put ourselves in a better situation to take care of our health in this new environment.








